Understanding Low Platelet Count
A low platelet count, clinically referred to as thrombocytopenia, occurs when the number of platelets in the blood falls below the expected physiological range. Platelets are small blood components produced in the bone marrow that play a critical role in preventing blood loss by assisting in clot formation at sites of vascular injury. When platelet levels are reduced, the body’s ability to control bleeding is compromised.
In adults, platelet counts below approximately 150,000 per microliter of blood are considered lower than normal. The clinical significance of thrombocytopenia varies depending on the degree of reduction and the presence of underlying medical conditions.
Physiological impact of low platelets
Platelets are central to the body’s haemostatic mechanisms. Reduced platelet numbers can impair clot formation, leading to delayed cessation of bleeding following minor injuries. As platelet levels decline further, the risk of bleeding from mucosal surfaces and internal organs increases. In severe cases, bleeding may occur without any apparent trauma, requiring urgent medical attention.
Mild thrombocytopenia may not produce noticeable symptoms and is often detected incidentally during routine blood investigations performed for unrelated medical reasons.
Clinical signs and symptoms
The manifestations of thrombocytopenia largely reflect impaired blood clotting. Common clinical features include:
- Easy or unexplained bruising
- Prolonged bleeding after cuts or minor procedures
- Recurrent nosebleeds or bleeding from the gums
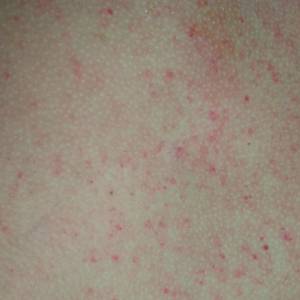
- Pinpoint red or purple spots on the skin (petechiae)
- Larger purplish skin patches due to subcutaneous bleeding (purpura)
- Blood in urine or stools
- Excessive menstrual bleeding in women
When platelet counts fall to very low levels, patients may also experience fatigue, dizziness, or signs of significant blood loss.
Underlying causes of thrombocytopenia
Low platelet levels can result from several pathophysiological mechanisms:
Reduced Platelet Production
Conditions that impair bone marrow function may limit platelet formation. These include bone marrow disorders, certain cancers, systemic infections, nutritional deficiencies, and the effects of chemotherapy or radiation therapy.
Increased Platelet Destruction
In some disorders, platelets are destroyed prematurely. This can occur in immune-mediated conditions where the body mistakenly targets its own platelets, as well as in certain thrombotic or inflammatory diseases.
Platelet Sequestration
An enlarged spleen may retain an excessive number of platelets, reducing their availability in the circulating blood.
Medication-Related Causes
Some medications can adversely affect platelet counts by interfering with production or increasing platelet destruction. Identifying drug-related causes is an important step in evaluation.
Diagnostic evaluation
Assessment of thrombocytopenia begins with a complete blood count (CBC) to confirm reduced platelet levels. Additional testing may include microscopic examination of a peripheral blood smear to assess platelet morphology and exclude laboratory artifacts. In selected cases, further investigations such as bone marrow examination may be required to determine the underlying cause.
A thorough medical history and medication review are essential components of diagnosis.
Management and treatment options
Treatment strategies are guided by the severity of thrombocytopenia, the presence of bleeding symptoms, and the underlying cause. Patients with mild, stable platelet reductions and no bleeding may only require periodic monitoring.
More significant cases may require targeted medical therapy, modification or discontinuation of causative medications, or treatment of underlying conditions. In emergency situations involving active bleeding or extremely low platelet counts, platelet transfusion may be necessary. Chronic or immune-related cases may require specialist-directed therapy.
Prognosis and follow-up
The outlook for individuals with thrombocytopenia varies widely. Many patients recover fully once the underlying cause is addressed, while others may require long-term monitoring or treatment. Regular follow-up with a healthcare professional is essential to ensure safe platelet levels and prevent complications.
